
Homo Sapiens has 46 chromosomes: 22 pairs of autosomes, and two sex chromosomes, X+X or X+Y. PGD tests human pre-embryos for the presence of the correct number of chromosomes 13,18,21,X and Y; any combination other than 13,13,18,18,21,21,X,X (Normal female) or 13,13,18,18,21,21,X,Y (Normal male) is considered ABNORMAL.
A monosomy (absence of one chromosome) of any autosome is lethal in humans, only a few babies with autosomal monosomy have survived beyond birth, with severe abnormatilites. TIley all had monosomy of chromosome 21.
A trisomy (one extra chromosome) can occur with any of the chromosomes. However, the most common is a trisomy of chromosome 21, leading to Down's syndrome. According to the latest National Vital Statistics report, in the year 2002 out of 3,993,973 births, 1,850 had Down syndrome and 1,253 had "other chromosomal anomalies". Among these "other chromosomal anomalies" the most common is an abnormal number of sex chromosomes. Per each 100,000 recognized human pregnancies, around 1,400 abort due to an abnormal number of sex chromosomes, about 100 boys born with Kleinfelter syndrome (instead of XY have XXY, XXXY, XXYY, or even XXXXY sets of sex chromosomes) and about 50 girls born with Turner syndrome (instead of XX have X, XXX, or XXXX).
Apart trom chromosome 21, the only other autosomal trisomies with any significant frequency in newborn are trisomies 18 (Edward's syndrome) and 13 (Patau's syndrome); frequencies of either syndrome range from one in 2,000 to one in 15,000.
Apart from these five chromosomes (13, 18, 21, X, Y), the only other chromosomes noticeably affecting the outcome of established pregnancies are chromosomes 16 (trisomy 16 found in 1,229 among 15,000 spontaneous abortions) and 22 (extra copy was present in 424 out of 15,000 spontaneous abortions). These embryos never reach term, but they affect the outcome of hurnan pregnancies.
Aneuploidy for any other chromosome is lethal at the very first stages of embryo development, before a pregnancy can even be established.
Interpretation of the Results
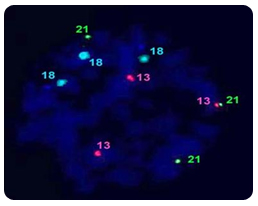
Triploid, tetraploid, or polyploid embryos are those having full extra sets of all 23 chromosomes. These embryos originate from an oocyte fertilized by two spennatozoa, by diploid spermatozoon, or from an oocyte which failed to extrude the second polar body. Polyploidization also occurs during embryo cleavage; at the blastocyst stage it is a normal step in trophectoderm formation. Haploid embryos originate trom parthenogenetically activated oocytes; they have only one set of23 maternal chromosomes.
Any combination of auto somes other than normal (disomy), monosomy or trisomy will be called complex abnormality. These reveal some very serious errors in oocyte maturation and/or embryo cleavage. Chaotic embryo cleavage is the most probable mechanism by which complex chromosomal abnormalities may originate. Chaotic cleavage means that during mitosis, when the zygote and, subsequently, blastomeres divide into two daughter cells, the chromosomes segregate between two sister blastomeres randomly or chaotically. Most of these embryos are also morphologically abnormal and very few of them progress beyond the cleavage stage. Such embryos should not be considered for transfer.
If more than one cell is analyzed from an individual embryo (marked in PGD Report as a), b), ...), and conflicting results are obtained, this may be an indication of a FISH error (see below) or embryo mosaicism. Embryo mosaicism may be considered as a "mild" case of chaotic cleavage. Mosaicism is a result of mitotic error and as such arises during embryo cleavage, when one of the blastomeres divides into two genetically unequal 'daughter blastomeres'. This may lead to an embryo having both normal and abnormal cells, i.e., mosaic embryo. If an embryo is suspected of having genetically normal cells and cells with autosomal monosomy, such embryos should be AVOIDED during embryo transfer. Monosomic cells may be selected out during further embryo development; however, if their population rises above some critical level, the embryo dies before or shortly after implantation, like any other embryo with autosomal monosomy. Since chromosome 21 is an exception (see above), mosaic embryos with monosomy 21 should not be considered for transfer.
If an embryo is suspected to have genetically normal cells and cells with autosomal trisomy, such embryos may develop into an abnormal mosaic baby. Some newborns with Down's, Edward's, and Patau's syndrome are actually mosaics. Mosaic embryos with trisomies should never be considered for transfer.
Some embryos may be revealed as abnormal even prior to FISH, during embryo biopsy or after blastomere fixation. If a single blastomere has more then one nucleus, it is called a multinucleate blastomere. Even if each nucleus (separated in PGD Report by [...]) is genetically normal, or if they add to a normal set of chromosomes, the corresponding embryo may be genetically abnormal. Multinucleation indicates some gross abnormalities in the timing between cell division, cytokinesis and nuclear division, karyokinesis. If cleavage results in one blastomere retaining both nuclei, then it's 'sister blastomere', will have none. Absence of a nucleus (anucleate blastomere) may be similar in its origins to multinucleation, but it may also be considered as an extreme example of embryo fragmentation. Although anucleate blastomeres cannot give any indications as to the embryo genetic background, it should be noted that their presence lowers embryo viability.
If multiple morphologically normal blastomeres were analyzed, and none of them had a nucleus, such an embryo may be considered 'not viable' due to gross errors in embryo cleavage.
Current estimates of FISH errors fluctuate around 10% for the detection of autosomal numerical abnormalities, and around 0% for sex determination. Due to the standard practice: "if not proven normal means abnormal", the rate of actual misdiagnosis is significantly lower. However, PGD technique cannot reveal all cases of embryo mosaicism, and for this reason, prenatal diagnosis via CVS or amniocentesis is strongly recommended.