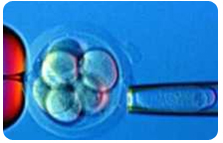
With current progress in understanding of the molecular basis of cancers, and sequencing of the genes involved in malignancy, inherited cancer predisposition became one of the emerging indications for PGD. Using a standard IVF procedure, oocytes or embryos can be tested for different mutations predisposing to cancer, preselecting and transferring only mutation-free embryos back to the patients.
The use of PGD to screen out embryos carrying a mutation predisposing to cancer, prevents the birth of children who would face a greatly increased lifetime risk of cancer, and hence require close monitoring, prophylactic surgery, or other preventive measures. Although these indications do not involve diseases that manifest themselves in infancy or childhood, the conditions in question lead to substantial health problems for offspring in their thirties or forties. Avoiding the birth of children with those conditions thus reflects the desire of parents to have offspring with good prospects for an average life span.
Prenatal diagnosis (PND) and selective pregnancy termination for adult-onset disorders is emotionally difficult and, in some cases, socially not well accepted. Preimplantation genetic diagnosis (PGD) appears as an attractive alternative to prenatal diagnosis, as it ensures the establishment of a pregnancy free of the mutation from the onset, circumventing the potentially difficult decision of termination of pregnancy.
Owing to the adult onset of hereditary cancer, prenatal diagnosis raises numerous ethical issues on the acceptability to terminate an affected pregnancy (TOP). This is the reason why prenatal diagnosis for these disorders is often considered as unacceptable by couples as well as geneticists and legal or ethical authorities. PGD for hereditary cancer, even if subject to controversy, seems to be a more acceptable option because it does not lead to TOP but consists of selecting embryos free from the mutation. Therefore, many couples, who do not want to transmit their cancer predisposition to their children, consider PGD as their only reproductive option.
People choose to have PGD for several reasons:
- it ensures that the child will not develop the inherited condition that is present in the family
- it avoids having to have a termination of an established pregnancy (many people choose to have PGD after already having several terminations of affected pregnancies)
For some people who have a moral objection to terminations, having PGD is a suitable alternative. However because of the problems associated generally with IVF treatments, PGD has some disadvantages.
IVF associated risks:
- invasiveness of treatment;
- cost of treatment – this is sometimes covered by the National Health Service (NHS);
- risk of not getting pregnant;
- increased risk of a multiple birth
- risks of ovarian hyper-stimulation syndrome (OHSS) caused by the drugs taken to stimulate egg production.
PGD specific risks:
- chance of inconclusive or incorrect test result;
- theoretical long-term risk to the person born following PGD.
Through PGD, couples with a familial history of cancer where one partner has the high risk gene now have an opportunity to start a pregnancy knowing that their offspring will not carry the cancer-predisposing gene mutation. DNA testing will be important to determine the genetic basis of the familial cancer so that a strategy to diagnose the mutation unequivocally can be designed by the PGD laboratory.
Genetic counselling to review the family’s genetic history and determine lifetime risk for that cancer will be an important first step in the decision-making process. Even if the risk is high, the decision to proceed with IVF and PGD will be a difficult one, particularly for fertile couples.
This will depend on the moral and ethical values of the couple, but also on their personal experience of cancer in the family. Couples will also be mindful of the advances in therapies for malignancies and that new and more effective treatments will become available in the future.
To complicate matters further, there are likely to be legal issues surrounding PGD for genetic predisposition to disease that will vary from state to state and country to country.